The Silver Bullet Blog
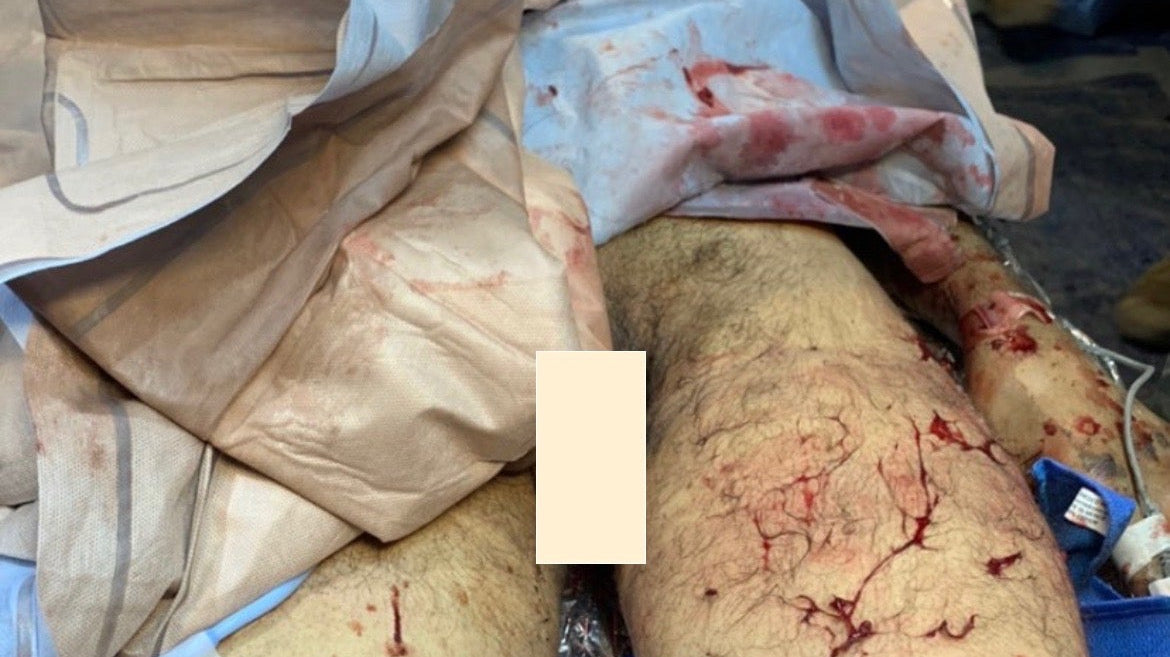
Double Amputation done by Special Forces Medic!
What makes a Special Forces Medic (18D) different from conventional Army Medics (68W’s)? It mostly comes down to prolonged field care—the ability to keep someone alive during a period of...
Life on an SF ODA-sorta
The majority of the over 2000 responses to our Instagram poll requested we talk more about life on a team and team deployments. We’ll eventually hit all the topics, but...
Mass Casualty Incident!!
Responding to a Mass Casualty Incident Awhile back, we had the massive explosion in Lebanon. More recently, we had the horrific explosion in Kabul that claimed the lives of 13...
The Misadventures of an 18D
The misadventures of an 18D across the world. It’s easy to forget that between the cool guy pics and polished image of many social media accounts, we’re all just normal...
Managing Junctional Hemorrhage
We are honored to share a guest write-up by Rob, @rob_o_medic, Senior 18D and instructor on the treatment of junctional injuries! ________________________________________________________________________ The hemorrhage that takes place when a main...
FAQ About Special Forces Assessment and Selection
Every day we receive numerous emails and messages on our page regarding questions about SF Selection (SFAS), the 18D course, and more. We love hearing from you all, but it...
FAQ on 68W/SOCM/18D and being a medic
We get asked multiple times a week if we have any advice to give for new 68w, those going to the SOCM course, or those interested in being a medic....
Heat Casualties
Heat Injuries! During a hospital rotation with the 18D course, I was working in the ER when a soldier was brought in with a core temperature of 108 degrees. We...
The Physics of a Gun Shot Wound
Anatomy and Physics of a Gunshot Wound (GSW) Gunshot wounds can be devastating. From the immediate impact on the organs of the body to their long-term consequences and lengthy recovery...
The Misadventures of Private Pea Brain
The Adventures of Private Peabrain In every unit, there is always inevitably going to be ‘that guy’. The one who tries his or her best, but inevitably just fails miserably...
SFAS Part 2: From Darkness until the Dawn
After my horrible and embarrassing attempt at the land navigation STAR course (if you haven’t read that debacle, feel free to refresh HERE), we moved into the dreaded team week...
When to Convert A Tourniquet
Tourniquet Conversion: Once again, we are blown away with the discussion that took place in regard to the question in our post about when and how to convert a tourniquet....